Displaying items by tag: foot health
Heel Pain: What Causes It and How To Treat It
Very few adults are strangers to heel pain. At some point in our lives, we've run too hard, hiked too far, gained too much weight, played basketball in past-their-prime sneakers, or didn't rest when we should have. Sometimes it even appears for no reason we can pinpoint. But without a doubt, we never forget that pinching and excruciating pain in our heel.

Heel pain occurs in the underside or the back of your heel. When it appears on the underside, it's usually a result of damage or irritation to the plantar fascia, the tendon which runs from your heel to the base of your toes. This type of heel pain is called plantar fasciitis. If heel pain occurs at the back of your heel, the cause is usually damage to the Achilles tendon, such as achilles tendinitis. But heel pain can also be caused by arthritis, a bruise, heel spurs, gout, pinched nerve, bursitis ("pump bump"), peripheral neuropathy, a fracture, bone infection, or other conditions. For this reason, any heel pain should always be evaluated by a podiatrist to determine the best course of treatment to get you back on your feet as soon as possible.
Schedule an appointment with a podiatrist if:
- You have severe pain and swelling near your heel
- Severe heel pain after an injury
- Inability to bend your foot downward without pain
- Inability to rise on your toes without heel pain
- Inability to walk without heel pain
- Heel pain that continues when at rest
- Heel pain that lasts more than 1 week
How to treat heel pain at home
Rest, Ice, and Elevation. Ice packs on the heel reduce inflammation, especially when paired with over the counter anti inflammatory medicine like advil or aleve. Rest and elevate the sore foot whenever possible.
Change your routine. If heel pain is the result of an athletic injury, change your routine. Training the same way, on the same surface, with the same shoes, will only make things worse.
Stretch before working out. Stretching your feet, raising yourself on your toes, even walking, will help warm up the plantar fascia and achilles tendon, reducing the risk of injury. When muscles, tendons, bones, and joints are gently warmed up before a workout, they're much better at handling the load you demand of them.
Are you wearing a quality pair of shoes? Whether athletic shoes or dress shoes, your footwear must fit your feet correctly and give ample support and padding. You may save money with cheap shoes, but the pain will be expensive.
How a podiatrist may treat your heel pain
- Custom orthotics to support your feet and relieve pressure on the heel
- Shoe modifications
- Prescription medications
- Steroid injections to relieve pain and inflammation
- Immobilization in a walking boot
- Physical therapy
- If conservative measures are unsuccessful, surgery may be recommended
Read more: Does your child have heel pain?
Pain In Your Big Toe? You May Have A Bunion
You have pain in your big toe, the joint below your big toe is sore and stiff and a bump protrudes from the side of your foot, frequently ruining your footwear. You may have just discovered a bunion.
[caption id="attachment_5040" align="alignleft" width="360"] The protrusion at the base of the big toe is a bunion.[/caption]
The protrusion at the base of the big toe is a bunion.[/caption]
Do shoes cause bunions?
It's commonly thought that high heels and other non-flat footwear are the cause of bunions. While these shoes aren't the primary reason for developing a bunion, they definitely contribute to their severity.
The truth is, some women can wear high heels their entire lives and never develop a bunion. Others can make all the right choices in footwear and still develop them. That's because the foot structure which contributes to a bunion is an inherited trait, especially common in men and women of European descent (but especially women). Any podiatric surgeon will tell you that he/she has treated bunions in multiple generations of the same family - usually mothers and daughters.
Our feet are designed to carry our body weight evenly across all planes of the foot. When we inherit the faulty biomechanics which lead to a bunion, and then stuff our feet into high heels and other shoes which don't support our feet correctly, a bad situation gets even worse. Shoes with heels shift our body weight onto the front of the foot, placing stress on an already weakened joint. Other factors which may contribute to bunions are obesity, spending lots of time on hard surfaces (like factory floors), jobs that demand a lot of time on your feet, and hormonal changes.
Will a bunion get better on its own?
What you see protruding from the side of your foot is a deformity of the joint at the base of the toe. The first metatarsal bone (the longest bone in the foot) has turned outward and the big toe has been pulled toward the other toes, causing the head of the metatarsal to protrude. As footwear rubs against this area, or body weight is shifted onto this joint via shoes with heels, the bursa which cushions and protects the joint becomes inflamed and sore, and the joint becomes stiff. The misalignment and compromised foot structure also causes pain on the side of your foot or in your arch, and pain and discomfort in the adjacent toes.
Unfortunately, a bunion is a progressive condition, which means it won't get better on its own. The longer you wait to treat the bunion, the worse it will become. There are stretching exercises and other therapies you can use to reduce the pain and progression of the bunion, but the only way to restore your foot to its pre-bunion condition is with bunion surgery.
What to do when you discover a bunion
- Stop wearing high heels or any other kind of shoes which don't support your feet correctly. This also includes inexpensive dress shoes (don't cheap-out in this department, guys!)
- When at all possible, wear a high quality pair of athletic shoes which cushion your feet and provide proper arch support
- Don't wear shoes that are too tight or pointed at the toes - opt for a wide toe box and a wider shoe in general
- See a podiatrist right away to establish a baseline. A podiatrist can treat your bunion with non-surgical measures like stretching exercises to reduce bunion pain, bunion splints, toe spacers or custom orthotics.
The faulty biomechanics that cause a bunion also contribute to other foot conditions as well, such as hammer toes, overlapping toes, corns, and ingrown toenails.
Why Our Toenails Thicken As We Age
Many of our podiatry patients remark on how thick their toenails become as they enter (and pass) middle age. Their toenails become notably tougher to trim, which makes the possibility of cuts to the skin around the nails a real possibility. Thickened toenails also splinter easily.
[caption id="attachment_4884" align="alignleft" width="300"]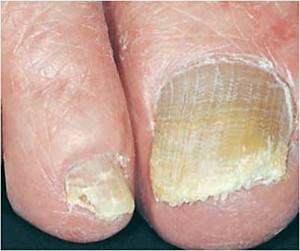 Toenails thicken due to aging, but other factors may also be at play.[/caption]
Toenails thicken due to aging, but other factors may also be at play.[/caption]
Unfortunately, thickening toenails are a by-product of aging, in most cases. As we age, our toenails - and fingernails - slow their growth rate, and the nails thicken because the nail cells, called onychocytes, sort of pile up. Fingernails appear to thicken less, probably because we tend to them more often with filing and buffing, which thins them.
But in addition to this natural thickening of the nails, other factors may be at play also. Among them are trauma, fungal infections, and impaired circulation. Feet are under constant stress from falling objects, stubbing injuries, poor foowear, closed-in footwear, and athletic activities. All of these conditions can alter the cells from which the nails grow, and if one tends to stub or injure the same toe, the nail plate can easily become thickened or disfigured.
Peripheral arterial disease, or P.A.D., a vascular disease which restricts blood flow to the extremities, can also cause thickened, brittle toenails. Fungus also plays a key role, as it thrives in the moist, dark interior of a shoe. Besides causing the toenail to thicken, a fungal infection may also cause the nail to yellow, become brittle, separate from the nail bed, and possibly emit a foul odor. In this case, your podiatrist may recommend trimming and cleaning (debridement) the toenail, a prescription topical creme or prescription oral medicine.
Reasons our toenails thicken
- Aging
- Fungal Infections (onychomycosis)
- Peripheral Arterial Disease
- Trauma
- Psoriasis (accompanied by red, scaly patches)
How to safely trim thickened toenails
**If you're diabetic, have peripheral arterial disease, or have diabetic peripheral neuropathy, a podiatrist should trim your toenails. Patients with these conditions frequently have a loss of sensation in the toes, and run the risk of wounding the skin or cutting too deeply when trimming the nails.
- Soften your toenails by soaking them in warm water for 10 minutes, then dry thoroughly.
- With a nail nipper, cut straight across the top of the toenail.
- Use small cuts straight across the toenail to avoid splintering, which may cause an infection.
- Do not round the toenails at the corner - this reduces your chance of developing an ingrown toenail
- With an emory board or nail file, gently file the edges of the cut toenail to remove sharp corners or edges which may catch on your sock.
Besides debridement, there are few treatment options to alleviate the thickening of toenails due to the natural course of aging. If however, your toenails are thickening due to one of the other causes mentioned above, your podiatrist will discuss a course of treatment with you.
Tips For Winter Foot Care
You may have looked at the title of this post and said, "put on thick socks!" And you'd be right - that's one tip to protect your feet from the cold this winter. But depending on your health, your lifestyle, and the condition of your feet, you might want to consider a few other tips for winter foot care as well.
[caption id="attachment_4769" align="alignleft" width="600"] A good pair of insulated boots and thermal socks are your feet's best defense against winter weather.[/caption]
A good pair of insulated boots and thermal socks are your feet's best defense against winter weather.[/caption]
Cold weather tips for diabetics
If you have type 1 or type 2 diabetes, you're at greater risk of foot injury during the winter months than you are at any other time of year. A side effect of diabetes called Diabetic Peripheral Neuropathy causes a loss of sensation in your feet, the result of persistently high blood sugar which damages blood vessels and nerves. DPN doesn't typically appear overnight - one experiences a slow loss of sensation over a period of years as the damage occurs. This makes a diabetic patient especially vulnerable to frostbite or frostnip, potentially damaging skin and other cells.
Diabetics - and everyone - should use common sense if they're going to be outdoors for a prolonged period. Keep moving to stimulate circulation, take breaks to warm up whenever possible, wear an excellent pair of waterproof boots, and wear 2 pair of thermal socks. Take an extra pair of socks with you in case your feet get wet. If your feet are icy cold to the touch, but you don't feel the appropriate sensation, you may have already developed DPN. Please make an appointment with your podiatrist immediately for an examination and treatment plan.
Cold weather tips for runners, hikers, skiiers, snowboarders, and all athletes
Just because you're moving, it doesn't mean you're invulnerable to freezing weather. In fact, splashing through wet streets, icy slopes, and getting your boots, socks, or sneakers wet, not only opens the door to a wicked wipeout, but also to frostbite or frostnip. Anyone who's spent significant time outdoors hiking, camping, sledding, or skiing is usually acutely aware of this from personal experience. But did you know that once you get frostbite or frostnip, you risk a more severe injury if it happens a second time?
[su_column][su_note note_color="#fff2f6" text_color="#ffffff" radius="3"]Learn to recognize the signs of frostbite (Mayo Clinic)[/su_note][/su_column]
Athletes should avoid training on wet surfaces, or at least splashing through puddles or snow. Hikers, campers, hunters, skiiers and snowboarders should have quality boots and appropriate socks to keep their feet warm and dry. If you notice a loss of sensation in your feet to any degree, get indoors immediately (or somewhere warm), take off your shoes and socks, dry your feet if wet, and allow your feet to slowly warm. If pain accompanies the warming, you may have frostnip. See a podiatrist for an evaluation.
Winter foot care for everyone
- Use common sense and keep your feet warm and dry.
- Wear comfortable, insulated boots that leave room for 2 pair of thermal socks. Your winter boots should also have a good sole to give you plenty of traction on wet surfaces.
- Wear thermal socks. If your feet are cold, wear 2 pair. Pass on cotton - choose synthetic fabrics that wick moisture away from your skin.
- If your feet tend to dry out in winter, moisturize them on a regular basis. But don't moisturize in between your toes - too much moisture in that area may lead to a fungal infection.
- Stay well hydrated to avoid chafing. This helps to prevent dry, cracked skin and blisters.
- Use talcum powder on your feet to keep them dry - good advice for any time of year.
